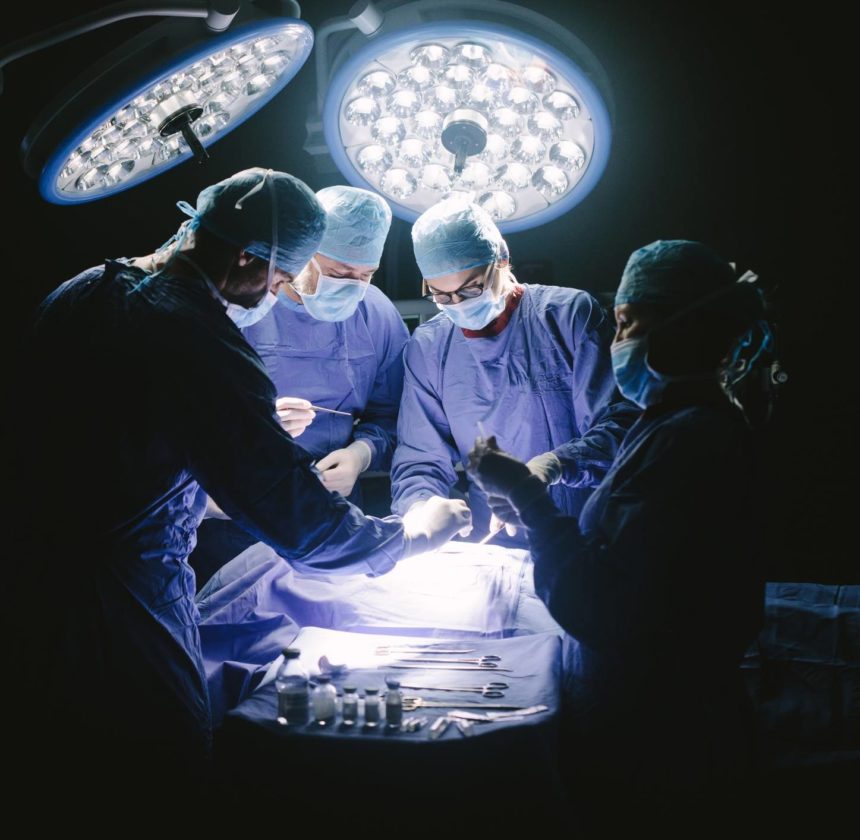
Anaphylaxis is a life-threatening medical emergency triggered by a severe allergic reaction to something that has entered the body. It might be something simple like a peanut, or it can be one of the components of a complex medication like the ones used as a general anaesthetic.
Many operations involve the administration of anaesthetic drugs immediately before surgery. These are usually given intravenously in combination and can include a synthetic opiate; muscle relaxants; antibiotics and anaesthetic induction agents. The prescription of these drugs will be managed by an Anaesthetist and should be documented in terms of timings and dosage on an anaesthetic chart and sometimes in the patient’s clinical notes.
Peri (meaning “during”) -operative anaphylaxis is the medical term for an allergic reaction that happens while someone is having surgery. Because the patient is unconscious and can’t explain what’s happening to them, it can be very dangerous if left untreated.
What precautions should be taken before surgery to prevent anaphylaxis?
Immediately before the operation the patient’s temperature; blood pressure, pulse, respiratory rate and oxygen saturations should be taken and recorded and during the anaesthetic induction and throughout the surgery the patient’s key stats should be monitored . These will be available on a clinical monitor which should be available both in the Anaesthetic room and Operation Theatre.
As allergic reactions tend to be more common when drugs are given intravenously (into the vein), every practitioner who gives drugs via this route needs to be able to recognise and treat such reactions quickly and appropriately.
Statistically, for every 2297 general anaesthetics given, only one will produce an allergic reaction. A National Audit Project (NAP6) found the first signs of the reaction were low blood pressure (46%), bronchospasm/high airway pressure (18%), rapid heart rate (9.8%), oxygen desaturation (4.7%), slow heart rate (3%) and reduced or absent capnography carbon dioxide trace (2.3%). Although rash was not always a presenting feature, this did develop in 56% of cases.
Common drugs that cause an allergic reaction during surgery
The commonest drugs to cause an allergic reaction during surgery were antibiotics, followed by neuromuscular muscle relaxants. The commonest antibiotic to cause a reaction was Co-Amoxiclav (Augmentin) whilst the commonest neuromuscular muscle relaxant causing anaphylaxis was Rocuronium.
Training in the treatment of anaphylaxis is a core component of the anaesthetic curriculum and every anaesthetist should be familiar with treatment protocols. It is important anaesthetists understand the signs of severe anaphylaxis since there are a wide number of other conditions that could share the symptoms, and there is no test which can produce a definite diagnosis. Anaesthetists should have regular simulation training to rehearse what to do in a severe allergy scenario to ensure timely and effective interventions are given.
Departments of Anaesthesia should have protocols for the detection, management and referral for investigation of peri-operative anaphylaxis. These should be readily accessible to all departmental members, widely disseminated and kept up to date. Clinical Directors of Anaesthetic Departments should ensure their anaesthetists have been trained in the management of perioperative anaphylaxis.
Why is anaphylaxis dangerous?
Anaphylaxis can rapidly develop into a life-threatening situation. The time for the allergic reaction to take place is less than five minutes in 66% of cases, less than ten minutes in 83%, less than 15 minutes in 88% and less than 30 minutes in 95% of cases as recorded (NAPP6).
The mortality rate associated with perioperative anaphylaxis has been estimated to be 4% in France, 3.8% in the UK and less in Australia and New Zealand.
Anaesthesia anaphylaxis treatment packs, including an anaphylaxis management algorithm, adrenaline pre-filled syringes suitable for IV administration, hydrocortisone and details of the location of Glucagon and Vasopressin are available, and should always be on hand where surgery is performed.
How is anaphylaxis treated?
Adrenaline is the primary treatment of anaphylaxis and should be administered immediately if anaphylaxis is suspected.
The aims of treatment for anaphylaxis are to support the organs of the body whilst waiting for the reaction to diminish. The beneficial effects of adrenaline in treating anaphylaxis are almost instantaneous; the blood pressure begins to increase in seconds. In the vast majority of patients, a good outcome should be achieved.
Where a critical peri-operative hypotension (low blood pressure) event occurs, and peri-operative anaphylaxis is one of the several differential diagnoses, treatment for anaphylaxis should start immediately as the reaction will often get worse as the immunological response heightens.
The rapidity of progression; potentially serious consequences if untreated; ease of and effectiveness of treatment are the main reasons why I believe that practitioners faced with the suspicion of anaphylaxis as a potential cause of low blood pressure and concerning clinical signs should err on the side of causation and treat as anaphylaxis. When under a general anaesthetic the patient can’t communicate of the signs themselves, so clinicians need to shoulder that responsibility on their behalf.
I’d like to see clinicians taking a more active approach to the diagnosis and treatment of anaphylaxis during surgery, as there is little to be lost and much to be gained.