A stroke is a serious and life-threatening condition caused when the blood supply to part of the brain is cut off or reduced, leading to rapid loss of brain function, This disruption in blood supply means the brain does not receive the essential oxygen it needs, which in turn causes the brain cells to die (this is known as hypoxic brain damage).
There are two main types of stroke. The most common is an Ischaemic Stroke – which accounts for around 85% of all strokes. An Ischaemic Stroke occurs when a blood clot travels to one of the arteries which supplies blood to the brain and gets stuck, blocking it and cutting off the blood and oxygen flow to the brain.
The second kind of a stroke is a Haemorrhagic Stroke, which occurs when a blood vessel bursts, causing a bleed on the brain. The burst blood vessel cannot carry blood to the brain cells as it should, starving them of oxygen and causing them to die.
There is no way to reverse the damage done to brain cells from the lack of oxygen and so the damage caused by a stroke can be permanent and, without urgent treatment, can lead to serious disability or death.
In this article we will explore ten of the most commonly asked questions about strokes.
1. How do you know if someone is having a stroke?
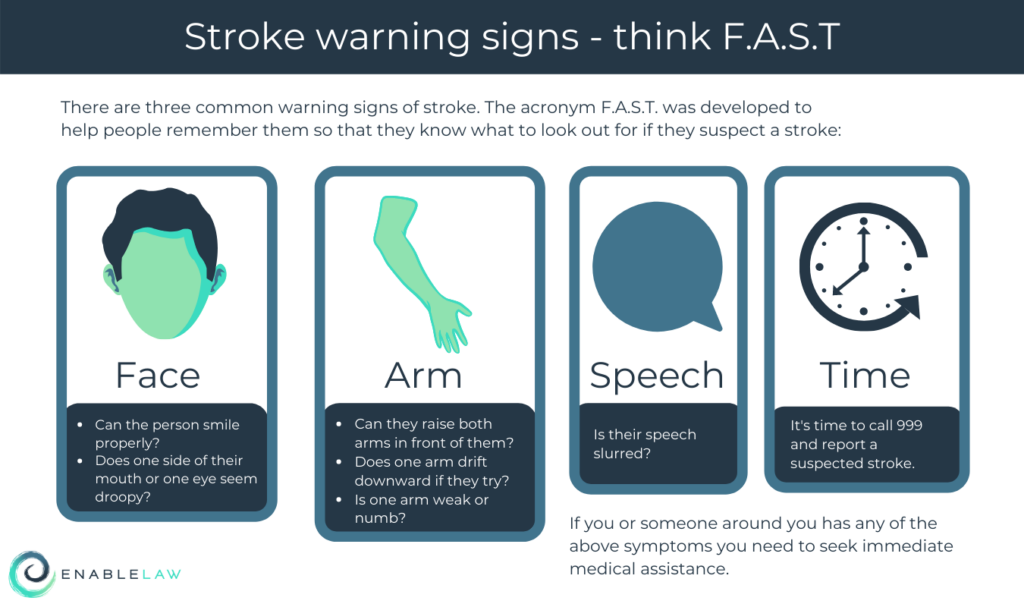
The initial symptoms can vary from person to person; but there are three common warning signs of stroke. The acronym F.A.S.T. was developed to help people remember these symptoms:
Face – In particular a facial droop. Can the person smile properly? Does one side of their mouth or one eye seem droopy?
Arms – Can they raise both arms in front of them? Does one arm drift downward if they try? Is one arm weak or numb?
Speech – Is their speech slurred?
Time – If you or someone around you is suffering from any of the above symptoms you need to seek immediate medical assistance. It’s time to call 999 and report a suspected stroke.
Other symptoms/early warning signs of stroke in adults can include:-
- A severe headache which comes on suddenly
- Blurred vision / sudden loss of vision
- Dizziness
- Confusion
- Difficulty swallowing
- Balance and co-ordination problems
- Difficulty understanding and communicating with others
- Paralysis of one side of the body
In children and babies some warning signs of stroke are the same as those seen in adults, but these may present differently and so it is important to aware of these, especially for babies and toddlers who are unable to communicate the difficulties they are experiencing. Stroke symptoms to look out for in infants and children include:
- Limb weakness, which may present as difficulty standing or walking (particularly on one side or stopping using a particular limb)
- Drowsiness
- Difficulty swallowing
- Increased dribbling
- Severe headache
- Behavioural changes
- Seizures
- Collapse
- Difficulty focusing eyes
If you notice any of these symptoms it is important to seek medical advice immediately.
2. What is a Mini Stroke?
A Transient Ischaemic Attack (TIA) is a condition which is related to stroke which occurs when the blood supply to the brain is interrupted temporarily. This condition is more commonly known as a “Mini Stroke”.
The symptoms of a TIA are the same as those of a stroke, however they tend to only last a few minutes to a few hours.
Although the symptoms pass TIAs should still be treated as a medical emergency as they often indicate that you are at significant risk of suffering from a full stroke in the near future.
3. Is it possible to have a Stroke and not realise it?
In short, yes.
It is possible to have what is known as a ‘Silent Stroke’, which is a stroke that you are either completely unaware of or have no memory of. Like ischaemic strokes, a silent stroke happens when the blood supply to part of your brain is cut off, however the typical warning signs of stroke (such as FAST) are not noticeable as the part of the brain which the stroke has disrupted the blood supply to is one which does not control motor functions (such as speech or movement); meaning there are no visible symptoms. Because of this it is possible you can have a stroke and not be aware of it. The most common way people discover they have suffered a silent stroke is by having an MRI or CT Scan for another condition. This could potentially be years after the event.
Unfortunately however, not being aware that you have had a stroke does not mean brain damage has not been caused. You may begin to suffer from cognitive symptoms such as memory loss, balance problems, frequent falls, mood swings, personality changes, laughing or crying at inappropriate times, bladder and/or bowel incontinence or difficulty with decision making. Research has also confirmed that suffering from multiple silent strokes puts a person at a significantly increased risk of developing vascular dementia.
4. How common is it to have a stroke?
Stroke is the most common non-traumatic cause of acquired brain injury. Around 100,000 people a year suffer from a stroke in the UK alone – that’s around one every five minutes; and in 2019 the World Health Organisation listed Stroke as the second highest single cause of death worldwide.
5. Who is at risk of having a stroke?
Ischaemic strokes, which are the most common kind, are caused by a blood clot blocking the flow of blood and oxygen to the brain. Whilst anyone can get a blood clot they are most likely to form in “clogged “arteries which have been narrowed over time by fat deposits. Arteries do naturally narrow as we age (which is why strokes are most common in older people) but the narrowing process can be sped up by certain things such as; diabetes, high cholesterol, smoking, hypertension (high blood pressure), obesity and excessive alcohol consumption.
Another cause of stroke is Atrial Fibrillation (AF), which is a condition which causes an irregular heartbeat. AF can cause blood clots to form in the heart which then travel to the brain causing a stroke.
It is a common misconception however that it is only older people who are at risk of stroke. Whilst it is true that majority of strokes occur in over 65s, anyone can be affected – from fit and healthy young adults, to children and even babies still in the womb.
Research has shown that in recent years more and more younger people are being affected by stroke, with 25% of strokes now occurring in under 65s and with stroke being in the top ten causes of childhood death.
6. Is it possible to prevent a stroke?
There are some lifestyle changes which can be made or pre-existing conditions which can be managed to help reduce your risk of suffering a stroke. These include; maintaining a healthy weight, stopping smoking, reducing your alcohol intake, and proper management and monitoring of ongoing conditions such as diabetes and hypertension.
7. How is a stroke diagnosed?
When a patient suspected of having a stroke arrives at the hospital, brain scans (typically either a CT scan or an MRI) will be taken in order to determine whether the stroke is an ischaemic stroke (caused by a blockage) or a haemorrhagic stroke (caused by a burst blood vessel). The scan will also help the doctors to establish how severe the stroke is and which area(s) of the brain have been affected.
Given the urgency of the situation the hospital will aim to ensure the scan is carried out within an hour of the patient arriving. Other investigations such as blood pressure checks and blood tests will also likely be carried out.
8. How is a stroke treated?
Stroke treatment varies depending on whether you have suffered from an ischaemic stroke or a haemorrhagic stroke. In both cases the sooner treatment is started the better the long-term outcome is likely to be.
Treating Ischaemic Strokes
Ischaemic strokes are most commonly treated with a mix of medications designed both to treat the condition and to prevent it from happening again. Some of the medicines will need to be taken short term, whilst others may need to be taken on an ongoing basis.
Thrombolysis (also known as “Clot Buster”) is another method of treatment for ischaemic strokes. It involves the injection of a drug called Alteplase into the patient. The Alteplase dissolves blood clots, which in turns restores proper blood flow to the brain.
Thrombolysis needs to be started as soon as possible after the stroke has occurred as if the stroke happened more than four and a half hours ago the use of Alteplase is no longer recommended. It is essential however for doctors to conduct a brain scan to confirm the patient has suffered an ischaemic stroke before starting thrombolysis treatment. If the patient had suffered from a haemorrhagic stroke the medicine would have the opposite effect and would worsen the bleed on the brain.
In severe ischaemic stroke cases brain surgery may be required. An emergency operation known as a Thrombectomy may be carried out in order to surgically remove the blood clot.
Treating Haemorrhagic Strokes
Emergency brain surgery may be required in order to treat a haemorrhagic stroke. The surgery, known as a craniotomy, removes the blood from the brain and repairs any burst blood vessels.
In some cases, a haemorrhagic stroke can cause a complication known as hydrocephalus. In these circumstances a tube (shunt) is surgically inserted into the brain to allow the fluid build-up to drain.
Following a haemorrhagic stroke you may need to take medication to lower your blood pressure in order to prevent further strokes.
9. What are the long-term effects of a stroke?
The impact of stroke can be devastating. Whilst some stroke survivors do make a good recovery, relatively quickly, many require significant long-term support.
Stroke can cause a number of both physical and cognitive symptoms including:-
- Paralysis
- Muscle weakness
- Communication difficulties, including the loss of the ability to speak
- Praxis (a reduced ability to carry out physical activities / movements)
- Difficulty swallowing
- Altered vision
- Loss of bladder and/or bowel control
- Loss of sexual function
- Memory loss
- Reduced executive function (such as the ability to problem solve, plan and reason)
Along with the physical and cognitive symptoms caused by the stroke many survivors also experience a significant psychological impact, most commonly experiencing symptoms anxiety and depression.
10. What help is available to help assist with stroke recovery?
Following a stroke an often-lengthy rehabilitation process begins to try to help survivors regain as much of their independence as possible. This support begins in the hospital and is continued in local clinics or at home.
The rehabilitation process varies from person to person and is dependent on the severity of the stroke and the symptoms they experience.
Often survivors will work with a team of specialists, dependent on their individual needs to help them to achieve the best recovery possible. These may include speech and language therapists, physiotherapists, occupational therapists and psychologists.
There are also a number of charities which work to support Stroke survivors and their families to help them going forwards. These include:
The Stroke Association – The only UK charity that focuses exclusively on stroke research. https://www.stroke.org.uk/
Different Strokes – The only UK based charity specialising in support for children and working age adults who have been affected by stroke. https://differentstrokes.co.uk/
Think Ahead – Founded in 2000 with the aim of improving the lives of stroke survivors and their families and carers. https://www.think-ahead.org.uk/
A Stroke of Luck – Specialising in exercised based rehabilitation by providing stroke survivors with the access to fitness professionals to aid their recovery. https://www.astrokeofluck.co.uk/
When might there be a clinical negligence claim after a stroke?
We receive many enquiries about stroke claims from survivors and their families concerning the treatment they have received.
In some cases the damage and injury caused by the stroke cannot be avoided. Occasionally however there may be situations in which a stroke may bring about a claim for clinical negligence. These include:-
- The failure to diagnose symptoms of a stroke;
- The failure to undertake appropriate investigations, such as MRI scans, leading to a delay in diagnosis;
- A delay in starting treatment;
- The delay in diagnosis or treatment of TIAs; And
- Failures to diagnose, monitor and/or treat underlying conditions which increase a person’s risk of stroke.
If you suspect that any of the above happened to either you or a loved one during their medical treatment, please contact us to find out how we can help.